A Brief History of Drug Delivery Methods
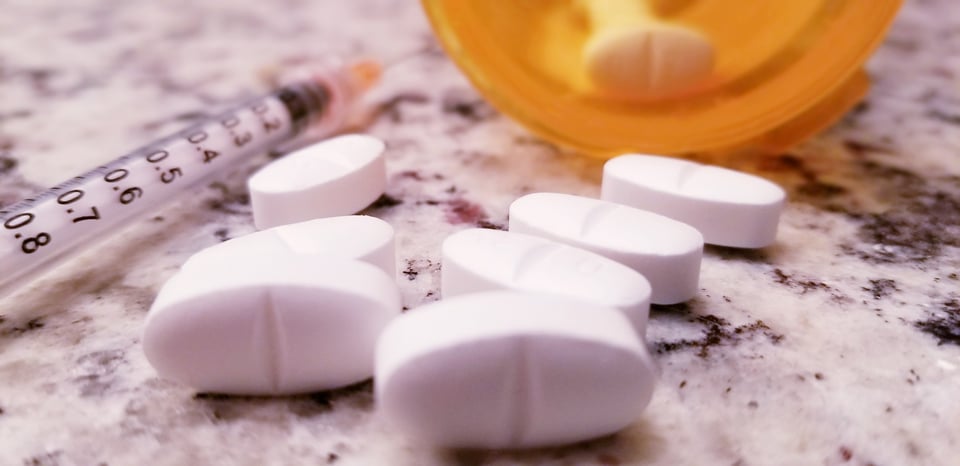
Accidental medical errors, specifically related to drug delivery and toxicity-related events, are the third largest cause of death among Americans, according to CNBC. More than 131 million adult Americans are making some sort of prescription medication in the form of an ingestible. Over 11.8 million people worldwide use an injectable device to deliver their medication daily. Now, the two devices that were mentioned, ingestible pills and the syringe needle used to inject medication, were invented in 1500 BCE and 1853 respectively. These forms of pharmacology delivery have not had dramatic changes since their inception into the world of medication. Even when taking into consideration medical safety, the largest changes in the form that these devices take have come from the inversion of the needle following injection and the “controlled-release” of medication from the pill form.
The slowed and “controlled-release” that the pill takes on comes from a slowly digestible lining of the physical pill that houses the active ingredients needed to make a physiological effect on the body. This has probably been the most recent development in the physician form that drugs can take, being patented in the late 1940s. It is rather astounding and difficult to attempt to conceptualize that in a field that pushes the boundaries in what is possible like pharmacology, that the delivery systems that are being used have not had drastic changes or innovations in hundreds of years. Leading some to argue, “why fix it if it’s not broken, right?” Well, that is the thing. It is broken, and it desperately needs fixing.
Needles, Pills, and Toxicity
Toxicity is the biggest fear of any prescribing physician or pharmacist that is giving a drug that needs to be highly regulated and have its dosage requirements strictly followed. The cause of death following an overdose of prescribed drugs is actually much more common in the United States than you may think. For example, as identified by the Centers for Disease Control and Prevention (CDC), from 1999 to 2019, nearly 247,000 people died in the United States from overdoses involving prescription opioids.
Toxicity is easily caused when using either an ingestible or an injectable device to deliver medication if there are even the slightest of errors. This toxicity can lead to disruption of central nervous function which in turn may cause mental disorders, damage the blood constituents, and may damage the lungs, liver, kidneys, and other vital organs promoting several disease conditions and even death. Understanding that dosage requirements are extremely strict for a reason is the beginning to understanding that our drug delivery system is extremely broken and in desperate need of innovative solutions that not only keep the patient safe, but that allow for physicians to make necessary adjustments to the regimen to deliver the best possible outcomes.
Doctors from the Tufts University School of Medicine and the Johns Hopkins School of Medicine concur that toxicity following mis-dosage of prescription medication, whether it be injected or ingested can cause extreme harm and can be avoided if physician intervention and monitoring were possible. There are several companies out there currently that are taking real-time data monitoring to the next level. The University of Colorado Health System, also known as UCHealth, is leading this charge in physician intervention. Dr. Richard Zane, Chief Innovation Officer at UCHealth, recently spoke on the podcast “Who Would Have Thought” and mentioned how some of the most promising technology in healthcare innovation is how “intelligence and automation and technology can be brought into monitoring workflows.”
"Thinking about how we can embed predictive and prescriptive analytics into decision making and present a provider with more information and better guidance."
Dr. Richard Zane, UC Health, Chief Innovation Officer
There is a need to change the way we are delivering medication and how our medical professionals can engage with our patient populations to ensure meaningful and efficient drug delivery to improve outcomes.
.png?width=1080&name=Crohns-Smarttab%20(2).png)
Newest Innovations in Drug Delivery
From the inception of the ingestible pill in 1500 BCE, which was made from bread dough, honey, or grease and filled with botanicals or animal parts and blood, the medication was delivered directly to the area where the outer shell was dissolved: the stomach. And, although this has been relatively helpful in the delivery of drugs that need highly vascularized areas to absorb their active ingredients, what about targeted drug delivery?
Sure, maybe the grease and tar that covered small pills that had small amounts of botanicals in the years of 100-200 AD would begin to dissolve shortly after the stomach, if at all, but bowel obstruction was common and often led to death. The targeted delivery of medication to the small and large intestines was basically impossible unless either injected directly, surgically intervened or if there was a pill taken with a battery-operated release mechanism that was usually unpassable.
Now, a company named SmartTab is developing a battery-free pill, TargetTab™, which is able to open directly where the medication is needed, no matter where in the G.I. tract, and give biometric data back to the physician in real-time. They're also creating another ingestible device that rids the need of needles, the largest cause of accidental prescription drug overdose, called the InjectTab™, that directly injects medication into the lining of the stomach and releases the optimal amount of drug painlessly.
There are also companies that use technology to remove needles from our everyday life like PharmaJet, which uses highly pressurized, extremely thin lines of liquid medication to penetrate the skin in a painless and controlled alternative to the needle. The amounts of medication are prescribed by physicians, but can only be delivered in the clinic rather than at the home of the patient.

Fixing a Broken Drug Delivery System
There is simply no need for human beings to die based on the inadvertent and accidental toxification of self or loved ones from prescription medication. We live in a world where a vaccine can be developed and approved by the FDA in under six months and be given to over 740 million people in an even shorter amount of time. Innovation efforts must be focused on how to better deliver medication so that it is more effective, safer to deliver, more accessible, and more readily available than it is right now. And it is possible - just look at the progress we make when faced with a challenge that we all believe can be overcome.
Resources & Citations
- http://tmrinternational.org/when-was-the-needle-was-invented/#:~:text=The%20hollow%20metal%20needle%20was,French%20surgeon%20Charles%20Gabriel%20Pravaz.
- https://www.targethealth.com/post/a-short-history-of-pills
- https://novel-drugdelivery-systems.pharmaceuticalconferences.com/middleeast/events-list/innovative-technologies-of-drug-delivery
- https://www.cnbc.com/2018/02/22/medical-errors-third-leading-cause-of-death-in-america.html
- https://www.avert.org/professionals/hiv-social-issues/key-affected-populations/people-inject-drugs
- https://hpi.georgetown.edu/rxdrugs/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6117810/
- https://www.intechopen.com/books/poisoning-in-the-modern-world-new-tricks-for-an-old-dog-/mechanism-and-health-effects-of-heavy-metal-toxicity-in-humans
- https://www.smarttab.co/
- https://pharmajet.com/stratis-imsc/
- https://ourworldindata.org/covid-vaccinations
.jpeg?width=1920&name=History%20of%20Innovative%20Drug%20Delivery%20Systems%20(1).jpeg)

